Rapidly spreading in the United States, this deadly fungal center | fungus | United States
According to the Associated Press on July 27th, in 2016, hospitals in New York State identified a rare and dangerous fungal infection that had never been detected before in the United States. The research laboratory quickly mobilized to retest historical specimens and found that this fungus has been present in the United States since at least 2013.
In the following years, New York City became the "explosive point" for ear Candida infections. According to data from the Centers for Disease Control and Prevention in the United States analyzed by the Associated Press, until 2021, New York State had the highest number of confirmed cases in the United States each year, but the disease has also spread to other places.
Candida albicans is a new global public health threat that may cause severe infections such as blood, wounds, and respiratory tract infections. Its mortality rate is estimated to be 30% to 60%, with a particularly high risk for individuals who have already suffered from serious illnesses and are being treated in medical institutions.
Last year, Nevada and California had the highest number of cases detected, but this fungus was found in patients in 29 states. New York State remains the main high-risk area.
Until 2009, no human body was found to carry Candida albicans. One theory that explains its sudden appearance is climate change.
The body temperature of humans and other mammals is higher than most fungal pathogens can withstand, so they have always been immune to most infections. However, rising temperatures may cause fungi to develop tolerance to warmer environments, and humans may also lose their protection over time. Some researchers believe that Candida in the ear belongs to this situation.
14 years ago, this pathogen coincidentally appeared on three continents, including Venezuela, India, and South Africa. Fungal disease expert, microbiologist, immunologist, and professor at Johns Hopkins University, Arturo Cassadwar, said this is puzzling because the climates in these places are completely different.
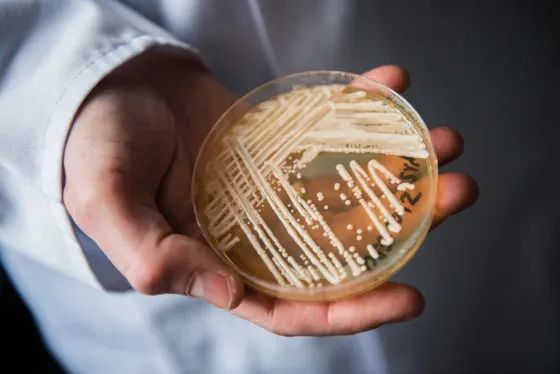
Candida samples from a laboratory in Werzburg, Germany
Kasadwal said, "Our body temperature gives us an extremely strong protective ability against fungi in the environment. However, if the world starts to warm and fungi also start to adapt to higher temperatures, some... will reach what I call the temperature barrier." He refers to the protective effect that mammalian body temperature has always had.
Meghan Mary Lehmann, an epidemiologist in charge of fungal diseases at the Centers for Disease Control and Prevention, said that when Candida albicans first spread, cases were all related to people traveling to the United States from other places. Nowadays, most cases originate locally and are usually transmitted among patients in medical settings.
Last year, there were 2377 confirmed cases in the United States, an increase of more than 12 times compared to 2017. However, Candida albicans is becoming a global problem. A survey last year found that from 2020 to 2021, the number of cases in Europe almost doubled.
Lehmann said, "There has been an increase in cases, but the geographical distribution has also expanded." She pointed out that although screening and monitoring have improved, the surge in cases indicates that the situation is still developing.
In March of this year, a press release from the Centers for Disease Control and Prevention pointed out the severity of the problem, stating that this pathogen is resistant to traditional antifungal therapies and spreads at an astonishing rate. Public health institutions are currently focusing on strategies to quickly alleviate the spread of this fungus in medical environments.
Lehmann said, "They are trying to extinguish a raging fire."
Dr. Louis Ostrowski, a professor of infectious diseases at the McGovern School of Medicine at the University of Texas Houston Health Science Center, believes that Candida in the ear is a "nightmare like scenario.".
He said, "This is a pathogen that may have multiple drug resistance and can spread rapidly in medical environments. We have never encountered such a pathogen in the field of fungal infections."
It has resistance to almost all the most commonly used antifungal drugs, and sometimes can also resist another drug mainly used to treat severe fungal infections in hospital catheters.
Ostrosky said, "I have encountered some cases where I sit down and face the families of patients, telling them that there is nothing we can do about this infection in your loved ones."
Osterosky treated about 10 patients with this fungal infection, but attended much more consultations. He said he had seen it infect the entire intensive care unit within two weeks.
Researchers, scholars, and public health organizations are discussing various theories to explain the emergence of Auriculococcus. Ostrosky said that climate change is the most widely accepted theory.
Lehmann from the Centers for Disease Control and Prevention said that this fungus may have been one of the microorganisms that live in the human body, but since it did not cause infection, it has not been studied until recently, causing health problems. She also said that there have been reports of the presence of this fungus in the natural environment, but environmental sampling has been limited and it is unclear whether these findings come from downstream human impacts.
She said, "There are still many problems related to increased contact with humans and human invasion of nature. In addition, there have been many changes in the use of fungi in the environment and agriculture. These situations may allow Candida to escape into new environments or expand their living space."




